 6 The authors of these studies concluded that lack of information contributed to the problems with administering drugs to patients on feeding tubes, and suggested that practice could be improved by involvement of pharmacists in establishing guidelines and training nurses. However, only 6.2 per cent of respondents listed pharmacists as their primary source of knowledge. Those who consulted pharmacy staff were more likely to use appropriate formulations and reported less obstructions of feeding tubes. In a survey carried out in the USA, 74 per cent of critical care nurse respondents used two or more inappropriate administration techniques for administering medications. Naysmith and Nicholson found that the majority of nurses surveyed were unaware of issues involved in giving a sustained release preparation of theophylline, few knew to stop feeds before and after giving NG phenytoin, and there was great variation in the volumes of diluent used to flush drugs down NG tubes. Despite this interest, several surveys have highlighted deficiencies in knowledge among nursing staff who routinely give drugs via a nasogastric (NG) tube, and practice has often developed by “trial and error”. The nursing profession has demonstrated a significant interest in this issue and this is reflected in the numerous publications discussing drug administration, particularly in enterally fed patients, and frequent requests for advice on this subject from pharmacy staff. 
In a study of all drug-related problems in 440 clinical nutrition patients, the most frequent problems related to drug interactions or incompatibilities with enteral or parenteral nutrition, and inappropriate administration techniques. General mechanisms of interactions between drugs and nutrients may include stimulation of blood flow to the splanchnic capillary network (increasing absorption), chelation of drug molecules by minerals such as calcium and iron, competing with the action of the drug (for example, vitamin K and warfarin), changing the pH of the gastrointestinal (GI) tract to increase or decrease absorption, blocking or enhancing metabolism and causing changes in gut motility to increase or decrease absorption. Drug effects such as drug-induced folate or vitamin B6 deficiency, drug-induced electrolyte imbalances, or effects of electrolyte imbalances on drugs, such as lithium may also need consideration. This article discusses how these challenges may be approached.ĭetails of the general effects of nutritional status on drugs are beyond the scope of this article, but factors such as concomitant disease states (renal failure, hepatic failure, short bowel syndrome), obesity or malnutrition can alter the pharmacokinetics or bioavailability of a medicine. The use of either the enteral or parenteral route provides pharmaceutical challenges in the delivery of medication usually delivered by the oral route. 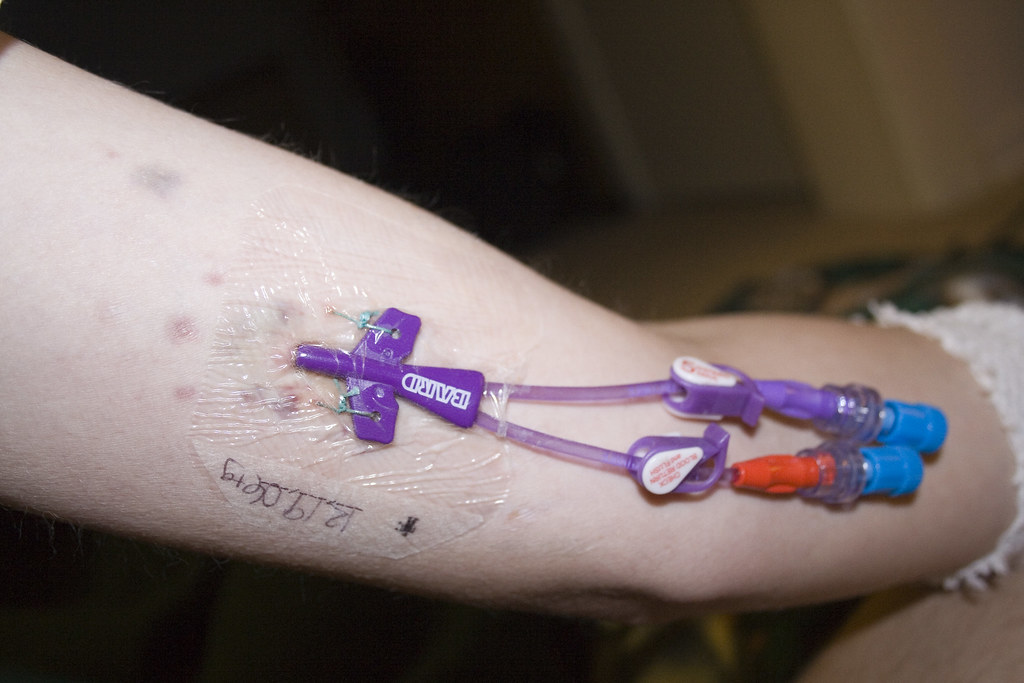
Patients with Crohn’s disease are an example of those who may need long term total parenteral nutrition (TPN). 
Both routes may be used for short term feeding in the acute setting or long term in the community. Nutritional status is now recognised to be an important part of medical care and nutritional support can be provided enterally or parenterally in various patient groups. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
